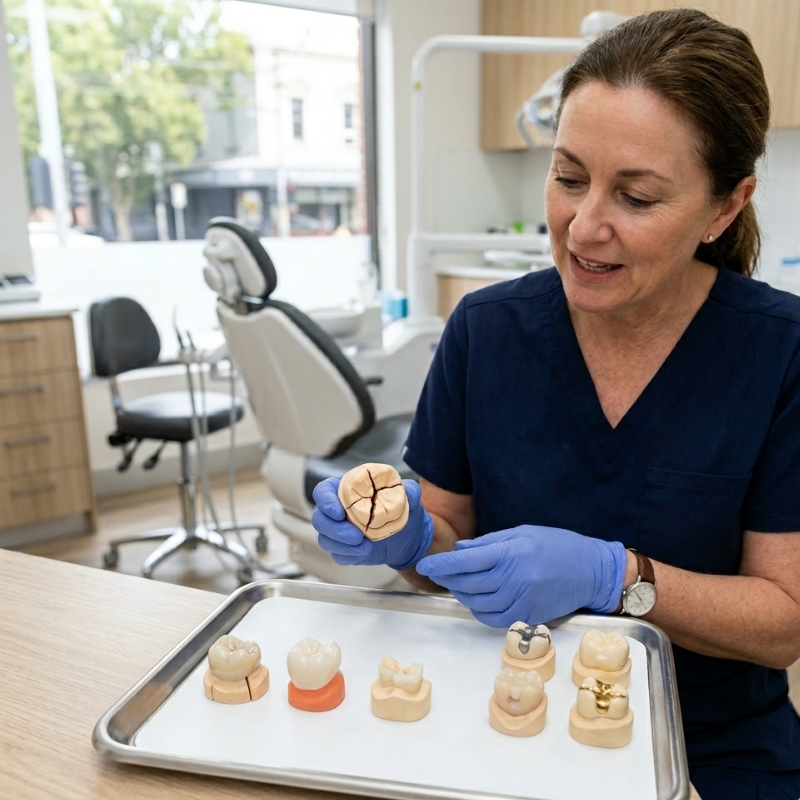
A cracked molar after biting down on an olive pit, a filling that keeps falling out, a front tooth that chipped during weekend footy — damaged teeth come in many forms, and the fix isn’t always obvious. While a full-coverage dental crown is one of the most reliable ways to restore strength, it isn’t automatically the right (or only) answer. Sometimes a well-placed filling, inlay, onlay or simple polish can protect the tooth without removing extra structure.
Below, you’ll learn how Melbourne dentists weigh up each option, what warning signs suggest a crown is safer, and the practical questions to ask before deciding. Use it as a starting point — then confirm the best path with your own clinician who can see the tooth in person.
1. Why Tooth Structure Matters More Than Pain Level
You can have a tooth that barely hurts yet is one bite away from splitting, or a tooth that aches thanks to a minor chip irritating the nerve. Pain alone isn’t enough to decide between a crown and a simpler fix. Dentists prioritise:
- Maintaining healthy enamel and dentine thickness
- Crack lines and fracture direction
- Existing filling size and integrity
- Proximity to the nerve (pulp)
- Bite forces (for example, heavier clenching at night)
- Location — front teeth usually face lower chewing loads than molars
In Melbourne’s modern restorative clinics, dentists often photograph cracks under high-magnification loupes or an intra-oral camera. These images help you see the hidden damage and understand why extra coverage might be recommended.
How a crown protects the structure
A crown acts like a 360-degree helmet, splinting weak walls together so they can handle daily chewing, coffee-to-cold-smoothie temperature swings, and occasional rogue popcorn kernels. Without that support, thin walls can flex and propagate cracks deeper into the root — a risk that fillings or inlays can’t always counter.
2. Early Warning Signs a Crown May Be the Safer Bet
Not every line across a tooth screams “crown me now”, but certain red flags push many Melbourne dentists toward full coverage sooner rather than later.
| Red Flag Sign | What It Often Indicates | Why a Crown Is Considered |
| Crack line visible on both sides of the tooth | Through-and-through fracture | Filling won’t stabilise flex; crown splints walls |
| Large existing filling >50 % tooth width | Remaining walls thin | The crown prevents further fracture under chewing load |
| Repeated filling failures in the same spot | Weak bonding surface or bite stress | Crown provides a stronger, indirect restoration |
| Tooth darkens after trauma | Possible pulpal damage, future brittleness | The crown can reinforce the post-root-canal tooth |
| Pain on release (biting then letting go) | Cracked Tooth Syndrome | Coverage redistributes forces across the cusp |
Pain when biting hard foods (nuts, ice), temperature sensitivity and food trapping can also point to hidden cracks. The sooner the tooth is stabilised, the better the long-term outlook.
3. When a Filling, Inlay or Onlay Can Still Work
Crowns require more tooth shaping and an extra appointment to fit. Where structure allows, Melbourne clinicians favour the least invasive option that still lasts.
- Small to medium cavities or chips: Modern bonded composites can restore shape and colour without heavy drilling.
- One or two thin cusps on an otherwise solid molar: A porcelain or zirconia onlay can cap the vulnerable cusp only, preserving healthy areas.
- Shallow vertical craze lines: Monitoring plus a surface seal may be enough if there’s no pain.
- Baby teeth or short-term solutions: Temporary fillings can buy time until growth or finances permit a crown.
If you’re on the fence, ask whether the tooth meets “onlay criteria” — enough surrounding enamel to bond to, minimal fracture risk and a bite pattern that won’t overload the repair.
4. Comparing Common Repair Options at a Glance
Some patients find the technical terms confusing. The table below summarises how each solution stacks up for strength, tooth preservation and appointment time.
| Repair Type | Best For | Tooth Structure Removed | Typical Strength vs Natural Tooth | Appointments Needed | Watch Outs |
| Composite filling | Small–medium cavities, front chips | Minimal (targets decay only) | ~60 % | 1 | May wear or stain over years |
| Ceramic/zirconia inlay | Medium cavity with intact cusps | Moderate | ~90 % | 2 | Limited if walls already thin |
| Ceramic/zirconia onlay | One or two weakened cusps | Moderate | ~100 % | 2 | Margins must sit on strong enamel |
| Full crown (all-ceramic or PFM) | Large fracture lines, post-root-canal teeth | Most (360° prep) | ~110 % | 2 | Requires healthy root structure |
| Interim stainless steel crown | Kids’ molars or emergency cover | Varies | Good short-term | 1 | Temporary aesthetics, replaced later |
PFM = porcelain fused to metal. Numbers are approximate relative strength comparisons to help visualise differences, not lab-measured guarantees.
5. Why Timing After a Root Canal Is Critical
Once infected pulp tissue is removed, the remaining tooth loses inner moisture and becomes more brittle. Most Melbourne endodontists advise full coverage within weeks, not months, to avoid catastrophic vertical fractures that can render the tooth non-savable.
The Australian Dental Association notes that post-endodontic cuspal coverage consistently improves survival rates for posterior teeth compared with fillings alone. You can review the ADA’s plain-language advice in their crowns resource.
In practical terms:
- Premolars and molars: Often crowned within 2–4 weeks of root canal completion.
- Front incisors: May cope longer with a bonded composite if little structure was lost, but full coverage still lengthens longevity.
- Temporary crowns: Protect the tooth while the final ceramic crown is made at a local dental lab. Avoid sticky lollies and floss sideways to keep it in place.
6. Case Snapshot: Hairline Crack vs Deep Split in Melbourne CBD
A 38-year-old accountant felt sharp pain when biting sourdough. Intra-oral photos showed a faint craze line on the upper molar. Bite-wing X-ray showed no split. The dentist opted for a bonded onlay, saving two cusps. Three years on, routine checks show no progression.
Contrast that with a Fitzroy café owner who delayed treating a visible crack. The fracture extended below gum level, splitting the root. Extraction and implant were the only options — a far more complex (and costly) pathway than an early crown would have been.
7. Questions to Ask Your Dentist Before Deciding
- How much healthy tooth is left after removing decay or the old filling?
- Are there visible or X-ray-confirmed cracks in the root?
- Will my bite pattern or grinding habits overload a filling or onlay?
- How long do you expect each option to last, assuming routine check-ups?
- What materials are available through Melbourne labs, and how quickly can they be made?
- If I try a less-invasive repair first, what signs mean I should convert to a crown later?
These questions steer the conversation toward structure and risk — not just cost or appearance.
8. Common Mistakes to Avoid
Ignoring Repeat Filling Failures
Each replacement thins the walls further. Three strikes often signal time for a stronger indirect restoration.
Delaying a Crown After Root Canal
Temporary fillings shrink and leak. Reinfection undoes endodontic work and hurts the wallet.
Weekend DIY Kits for Lost Fillings
Over-the-counter “cement” can plug a hole for 24 hours, but crowns need a precise shape and fit crafted by a dental lab.
Assuming Pain Level Equals Damage Level
Some of the worst fractures are silent until the tooth splits. Regular six-monthly exams catch changes early.
9. Which Option Fits Your Lifestyle?
- Busy professionals often prefer two-visit ceramic crowns or onlays over multiple repeat fillings.
• Contact-sport athletes might choose zirconia crowns for superior impact resistance, adding a custom mouthguard during AFL season.
• Cosmetic-focused patients lean toward all-ceramic solutions on visible teeth for natural translucency.
• Budget-conscious treatment plans sometimes stage care: stabilise with a filling now, crown next financial year once rebates reset.
Remember, a staged plan only works if the tooth has enough remaining strength to last that long without cracking.
10. Deciding When to Seek Professional Assessment
If you notice any of the following, book a timely exam instead of self-diagnosing:
- Sharp pain on release after chewing
- A visible dark crack running vertically
- Filling margins that feel “catchy” with floss
- Sensitivity worsening despite desensitising toothpaste
- A piece of tooth or filling breaking off
Not sure whether it’s urgent? See the practical pointers in our related resource on how to tell if a chipped tooth is serious. It walks through temporary measures and red-flag symptoms.
FAQs
1. Can I wait and see if the crack gets worse before crowning the tooth?
You can, but it’s a calculated risk. Minor craze lines sometimes stay stable for years, whereas deeper cracks can propagate suddenly. Monitoring should involve regular bite-wing X-rays and photos. Any increase in pain, widening of the line, or change in bite should trigger reconsideration of full coverage.
2. Do crowns weaken the tooth because they require extra drilling?
A small amount of additional enamel is removed to create space, but the finished crown splints the remaining walls together. Over decades, research shows crowned teeth often outlast large multi-surface fillings because they better distribute chewing forces.
3. Is zirconia always better than porcelain-fused-to-metal (PFM)?
Not automatically. Zirconia excels in strength and is metal-free, which helps gum health. PFM crowns, however, can be slimmer in areas with limited space and may still be chosen for back molars where aesthetics are less critical. Your dentist will weigh up space, bite and appearance.
4. What if I grind my teeth at night — will a crown just crack again?
Night-time clenching (bruxism) increases stress on any restoration. A custom night guard absorbs forces and protects crowns, fillings and natural enamel alike. Durable materials like monolithic zirconia further reduce fracture risk.
5. How long do crowns last?
Studies suggest well-made crowns last 10–15 years on average, with many exceeding 20 years when oral hygiene and bite forces are well managed. Regular six-monthly check-ups allow minor chips or cement wear to be fixed before they jeopardise the crown.
Final Thoughts
Choosing between a filling, inlay, onlay or crown rarely comes down to one factor. It’s a balance of remaining tooth structure, crack depth, bite forces and personal preferences around appointment time and longevity. A thorough clinical exam, clear photos and an honest discussion about risks will point you toward the safest solution for your individual tooth. If in doubt, seeking timely professional advice can prevent a small crack from becoming a bigger (and costlier) problem later on.